Intrapartum Care Skills PEARSON PDF

| Title | Intrapartum Care Skills PEARSON |
|---|---|
| Author | Jannine Voiles |
| Course | Family Health Concepts |
| Institution | Fayetteville Technical Community College |
| Pages | 6 |
| File Size | 251.7 KB |
| File Type | |
| Total Downloads | 99 |
| Total Views | 153 |
Summary
Intrapartum Care - amniotomy procedure, epidural anesthesia procedure, fetal external electric monitoring procedure, etc...
Description
NUR 113: Intrapartum Care Notes Amniotomy – a procedure that intentionally ruptures the amniotic sac to induce labor o
NOT delegated to UAP but can request the UAP to report pt observations for follow up
o
Must review MD’s orders and obtain signed informed consent from pt
o
Explain to the pt about the procedure - why it is necessary & how the pt can participate
*Assess fetal heart rate prior to, during, and following amniotomy because rupturing the amniotic membranes changes the pressure inside the uterus and causes risk of a prolapsed cord
During procedure – IMPORTANT! o
Once the membranes are ruptured and fluid is seen – note the color, amount, odor, and presence of meconium or blood
amniotic fluid should be clear or slightly cloudy & without any odor
meconium stained or bloody amniotic fluid places the fetus at risk for complications
foul smelling fluid may indicate an infection
absent, decreased, or increased amounts of amniotic fluid may indicate fetal stress
o
Maternal temperature should be assessed every 2h or more frequently if febrile and/or ordered
high temp might indicate intrauterine infection (chorioamnionitis)
Post-procedure: Document
Epidural anesthesia – used to lessen sensation in the lower body by blocking nerve impulses from the lower spine o
NOT delegated to the UAP but can request the UAP to report pt observations for follow up
o
Must review MD’s order and notify anesthesia personnel & obtain signed informed consent from pt
o
o
Explain about potential side effects (headache, hypotension)
Inform the pt that they should report the onset of a headache
Inform the pt of frequent blood pressure assessments
Explain to the pt about the procedure - why it is necessary & how the pt can participate
During procedure – IMPORTANT! o
Obtain maternal baseline VS, fetal heart rate, and variability
o
Administer an IV fluid bolus per facility policy before the epidural is begun to avoid hypotension
o
Assist and support the woman in position = side-lying with knees flexed or sitting up on side of bed with back flexed
o
BP, HR, and fetal HR are assessed before the test dose, every 5 min during the test dose and at the end of the test dose
o
Have ephedrine at bedside in case of hypotensive or fetal bradycardia episode
o
Assess the bladder for distention every 30 min because a full bladder can slow the descent of the fetus and risk damage to the bladder
o
Change positions at least every hour to maximize uteroplacental blood flow, increase circulation, promote comfort, and avoid a one-sided block
Post-procedure: Document
Fetal External Electronic Monitoring – used to listen to, see visual configurations, and record or print rhythm strips of the fetal heartbeat through the abdomen of the mother o
NOT delegated to the UAP but can request the UAP to report pt observations for follow up
o
Must review MD’s orders and explain to the pt about placing monitor belts around the abdomen – why it is necessary, how the pt can participate & how the results will be used in planning further care or treatments
During procedure – IMPORTANT! o
Have pt empty her bladder
o
Place the tocodynamometer (“toco”) over the uterine fundus off the midline on the area palpated to be firmest during contractions (the area of greatest contractility)
o
Resting tone tracing (without UC) = 10 or 15 mmHg pressure line adjust the line to reflect this
o
Apply the ultrasonic gel to the diaphragm of the ultrasound transducer & place the diaphragm on the maternal abdomen in the midline between the umbilicus & the symphysis pubis
o
Listen for the FHR (will have a whip-like sound) & move the diaphragm laterally if necessary to obtain a stronger sound
o
When the FHR is located, attach the second elastic belt snugly to the transducer
*FHR tracing provides information about fetal status and response to the stress of labor nonreassuring characteristics allows prompt interventions
Post-procedure: Document
Fetal Heart Rate: Auscultating – provides information about the health of the fetus and how the fetus responds to changes in the uterus environment o
NOT delegated to the UAP but can request the UAP to report pt observations for follow up
o
Review MD’s orders and explain to the pt that you are going to listen to the FHR using a Doppler – why it is necessary & how the pt can participate
During procedure – IMPORTANT! o
Check the pt’s pulse against the fetal sounds you hear – if the rates are the same, reposition the Doppler
If rates are not similar, count the FHR for 1 full minute (FHR has a double rhythm and only one sound is counted)
o
If FHR cannot be located, move the Doppler laterally
Auscultate the FHR between, during, and for 30 seconds following uterine contractions
Low-risk women: every 30 min in the first stage and every 15 min in the second stage
High-risk women: every 15 min in the first stage and every 5 min in the second stage
*FHR is heard most clearly through the fetal back. Locate the fetal back using the Leopold maneuvers
Fetal Internal Scalp Electrode Placement: Monitoring – (for better electronic monitoring of the FHR) electrode may be placed internally after the amniotic sac has ruptured & the cervix has opened during labor o
NOT delegated to the UAP but can request the UAP to report pt observations for follow up
o
Must review MD’s orders and obtain signed informed consent from pt
o
Pt’s membranes must have already ruptured spontaneously or been ruptured by the healthcare provider
Generalist RNs are not allowed to rupture membranes
During procedure – IMPORTANT! o
Explain the procedure, purpose, and implications of using a fetal scalp electrode to pt
o
Assist the pt into lithotomy position
o
Perform vaginal exam to determine dilation and presentation of the fetus
*Contraindications: membranes are not ruptured, the cervix is not dilated at least 2 cm, there is a reason a cervical examination cannot be done, there is a diagnosed infectious risk to the fetus, the presenting part is unknown, and the presenting part is not down against the cervix o
Apply fetal scalp electrode on a firm area of the fetal vertex (avoid fontanelles, face, genitals, etc)
o
Connect spiral electrode wire to a leg plate & secured by a self-adhesive grounding pad to the mother’s inner thigh
o
Verify FHR is tracing before discontinuing the intermittent or continuous external monitor
o
To remove disconnect the electrode wire from the cable & rotate the lead counterclockwise (once removed make sure it is intact)
Post-procedure
If unable to remove, tape electrode wire to the mother’s thigh and notify surgeon!...
Similar Free PDFs

Intrapartum Care Skills PEARSON
- 6 Pages

CPG-Intrapartum and Postpartum Care
- 98 Pages
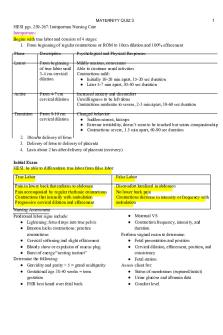

Quiz 3 HESI Intrapartum Care
- 8 Pages

Skills+Checklist+-+Wound+Care
- 2 Pages

Skills Checklist ostomy care
- 6 Pages

Prework intrapartum
- 2 Pages

P141 - Pearson
- 1 Pages

OB E2 - Labor and Intrapartum
- 38 Pages
Chapter 8-02 - Pearson - Homework
- 22 Pages

Chapter 8-01 - Pearson - Homework
- 15 Pages

Preoperative questions form Pearson
- 41 Pages
Popular Institutions
- Tinajero National High School - Annex
- Politeknik Caltex Riau
- Yokohama City University
- SGT University
- University of Al-Qadisiyah
- Divine Word College of Vigan
- Techniek College Rotterdam
- Universidade de Santiago
- Universiti Teknologi MARA Cawangan Johor Kampus Pasir Gudang
- Poltekkes Kemenkes Yogyakarta
- Baguio City National High School
- Colegio san marcos
- preparatoria uno
- Centro de Bachillerato Tecnológico Industrial y de Servicios No. 107
- Dalian Maritime University
- Quang Trung Secondary School
- Colegio Tecnológico en Informática
- Corporación Regional de Educación Superior
- Grupo CEDVA
- Dar Al Uloom University
- Centro de Estudios Preuniversitarios de la Universidad Nacional de Ingeniería
- 上智大学
- Aakash International School, Nuna Majara
- San Felipe Neri Catholic School
- Kang Chiao International School - New Taipei City
- Misamis Occidental National High School
- Institución Educativa Escuela Normal Juan Ladrilleros
- Kolehiyo ng Pantukan
- Batanes State College
- Instituto Continental
- Sekolah Menengah Kejuruan Kesehatan Kaltara (Tarakan)
- Colegio de La Inmaculada Concepcion - Cebu




