Wound Care Notes Wk 3 PDF

| Title | Wound Care Notes Wk 3 |
|---|---|
| Author | Alyssa Monique |
| Course | Advanced Wound Care |
| Institution | The University of Notre Dame (Australia) |
| Pages | 14 |
| File Size | 941.8 KB |
| File Type | |
| Total Downloads | 61 |
| Total Views | 152 |
Summary
The surgical wound & debridement & skin suture techniques...
Description
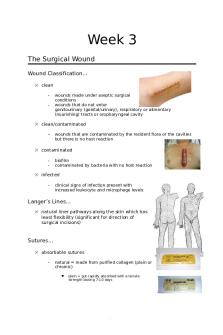
Week 3 The Surgical Wound Wound Classification… clean
wounds made under aseptic surgical conditions wounds that do not enter genitourinary (genital/urinary), respiratory or alimentary (nourishing) tracts or oropharyngeal cavity
clean/contaminated
wounds that are contaminated by the resident flora or the cavities but there is no host reaction
contaminated
biofilm contaminated by bacteria with no host reaction
infected
clinical signs of infection present with increased leukocyte and microphage levels
Langer’s Lines… natural liner pathways along the skin which has least flexibility (significant for direction of surgical incisions)
Sutures… absorbable sutures
natural = made from purified collagen (plain or chromic)
plain = gut rapidly absorbed with a tensile strength lasting 7-10 days
chromic = gut is treated with a chromium salt solution to resist body enzymes (prolonged absorption time of 10-14 days
Synthetic Sutures
absorbable
non-absorbable
polyglycolic acid (dexon) polyglactin (vicryl) polydioxone (PDS) polyglyconate (maxon)
polyamide (nylon) polyester (dacron) polypropylene (prolene)
vicryl
tensile strength ^ ^ ^
65% @ 14 days 40% @ 21 days 10% @ 35 days
absorption complete by 70 days
polydioxone
tensile strength ^ ^ ^
70% @ 14 days 50% @ 28 days 14% @ 56 days
absorption complete by 180 days
Wound Healing by Primary Intention… principles
protect the wound from physical or pathogenic assault absorb exudate maintain wound temperature maintain body temperature oxygenation avoid stress – pain relief
Dressing the Suture line… generally, only for 24-48 hours unless drains in situ
dry low-adherent dressings only eg:
Island dressings Semi-permeable film Hydrocolloid Foams
Surgical Wound Complications… types of complications:
haemorrhage – primary or secondary haematoma seroma oedema infection occlusion of blood supply - necrosis dehiscence sinus tracking evisceration adhesions
haemorrhage
primary = bleeding immediately following surgery secondary = bleeding that develops 24 hours + after the original injury/surgery (often caused by an infection or dislodged clot
fluid collection
seroma = a localised collection of serum within the tissues (contains blood plasma) oedema = excessive water in the tissues
sinus formation & tracking
sinus is cavity or track into the tissues aim is to heal the cavity from the base upwards in order to eliminate dead space in wound cavity wounds are gently packed to facilitate controlled wound closure
dehiscence
separation of tissue layers in a surgical wound generally as a result of infection, haematoma, fluid collection or local trauma
evisceration
protrusion of viscera or bowels through a surgical incision or traumatic wound keep covered with sterile moistened pads or drapes surgical emergency
fistula
a fistula is a track connecting one body cavity to another cavity or the skin surface can result from a leaking surgical anastomosis or spontaneous rupture due to obstruction, disease, trauma or radiotherapy damage a fistula can be internal or external types of fistulas:
Enterocutaneous (intestine – skin) - external Vesicovaginal (bladder – vagina) - internal Enterocolonic (intestine – colon) - internal Colocutaneous (colon – skin) - external Enterovaginal (intestine –vagina) - internal Colovesical (colon-bladder) - internal Rectovaginal (rectum-vagina) - internal Vesicocutaneous (bladder-skin) - external
assessment:
type of fluid identifies organs involved eg faeces, urine, saliva, gastric fluids, bile etc amount of fluid – high output >500 mls in 24 hrs, low output < 500 mls in 24 hrs. pH of fluid odour and gas X-ray with radio-opaque medium to identify position and tracking
Infection… clinical signs of wound infection
local:
pain heat oedema erythema (redness) exudate (change to purulent or increase amount)
systemic:
elevated temperature elevated leukocyte levels malaise
risk of infection
age (elderly or very young) aetiology – planned surgery, trauma number of comorbidities or control of same pre-op skin preparation peri-operative hypoxia, pain, anxiety, cold length of operation method of wound closure (bucknall, 1981 showed silk & braided sutures increased reaction) post-op care – infection control principles, wound drainage, dressings, shower, activity nutritional status
recommended dressing for restoring bacterial balance
Cadexomer iodine powder/paste, sheet dressing. Povidone iodine impregnated tulle gras Chlorhexidine impregnated tulle gras Wound honey Silver impregnated dressings Polyhexamethylene biguanide (PHMB) products.
Skin Grafts… what is it?
a skin graft is a segment of dermis and epidermis which has been completely separated from its blood supply and donor site attachment before being transplanted to another area of the body
types of skin grafts:
Autografts = transfer of tissue from one site to another on the same person. Allografts/Homografts = transfer of tissue from one person to another (eg skin, bone, organs).
Xenografts/Heterografts = transfer of tissue from one species to another (eg pig skin) Tissue Culture = epidermal cells cultured in the laboratory Bio-engineered Skin = Dermagraft, Apligraf
taking a skin graft
split thickness
can be thin, intermediate, or thick and contain all of epidermis and variable depth of dermis. thin = contracts within the first few months. No hair. Higher survival rate as vascularisation occurs easily. thick = less contraction. usually contains some hair follicles
full thickness
contains all of epidermis & dermis donor site has to be directly closed or grafted
factors which inhibit graft take
poorly vascularised recipient bed shearing movement fluid collection beneath the graft (eg haematoma, seroma, pus, debris) infection inadequate graft support when dependent patient factors
shearing forces
movement between the graft and the recipient bed causes damage to the capillaries growing into the graft and prevents revascularisation nursing interventions:
pain splinting (eg thermoplastic splints) patient education (eg keeping graft site immobilised) stabilised dressings (cotton tulle gras, silicon dressings, tie-over, compression)
fluid collections beneath the graft
good contact between the graft and the recipient bed is essential for vascularisation nursing interventions:
Seroma/Haematoma: regular graft care (dependent on exudate level), nicking/pricking any blisters that form, haemostasis if bleeding, evacuation of haematoma preparation of the recipient bed to remove non-viable tissue
infection
pre-graft recipient bed preparation post-grafting:
infection control aseptic technique infection results in increased exudate which lifts the graft off its bed
nursing interventions:
identification of signs and symptoms of infection compliance with the treatment plan if infected graft care: removal of accumulated exudate and crusts, trimming of graft once taken
Flaps… what is it?
flap is a surgical relocation of tissue from one p art of the body to another part in order to reconstruct a primary defect flaps are described as skin or cutaneous flaps and composite flaps
types of skin grafts:
skin or cutaneous consisting of skin and superficial fascia (small defects)
composite tissue:
fasciocutaneous flap (subcut tissue and deep fascia – more blood for larger defects) myocutaneous flap (layer of muscle – for bulk or functional muscle ) osteomyocutaneous flap (bone e.g. In jaw reconstruction)
free flap
relocation of skin & subcutaneous tis sue as a complete segment with an anastomosis of the blood supply
pedicle flap
a transfer of skin and tissue to another site blood supply to the flap is maintained via a vascular pedicle
rotational flap
a ‘Z-plasty’ used to free up tissue & rotate to an adjacent site
stabilisation
uses external fixators
flap observations
warmth - reduction in temperature change in tissue: prune-like or hollow if arterial occlusion. tense, swollen and distended if venous occlusion. skin colour changes bleeding decrease or increase in capillary refill time
nursing care
follow post-op orders observe vital signs, preferred range:
T, 36.5-37.5oC P, 100mm Hg
monitor fluid intake - IV and oral monitor urinary output, 0.5ml per Kg/hr oxygen therapy and continuous saturations maintain 96% or > observation of flaps observations of drains and dressings
donor sites
complications
nursing interventions
infection bleeding delayed healing
observation of donor site dressing donor site observation (eg pain, bleeding, malodour, cellulitis, purulent exudate) protect healed wound
donor site dressings
alginates hydrofibre hydrocolloids foams retention dressings (eg. fixomull)
Debridement What is it? … the removal of all foreign material and all
contaminated and devitalised tissue from or adjacent to a traumatic or infected lesion until healthy tissue is exposed
Necrotic Tissue … factors:
hinders assessment of tissue dama ge interferes with granulation inhibits wound contraction obstructs epithelial migration promotes bacterial proliferation may cause odour
Debridement Methods … use TIME CDST
surfactant surgical conservative sharp mechanical autolytic enzymatic chemical biological or parasitic ultrasound
surgical debridement
under aseptic conditions by surgeon
mechanical debridement
use of wet to dry dressing or irrigation under pressure
autolytic debridement
hydration of the wound to promote autolysis (destruction of cells or tissues by their own enzymes) of necrotic tissue eg. hydrogels, hydrocolloids
chemical debridement
cadexomer iodine wound honey hypertonic saline
biological/parasitic debridement
secrete collagenases & trypsin - extracorporeal digestion antimicrobial activity including Clostridium welchi ,MRSA & Pseudomonas slight pyrexia may result during lysis of bacteria by maggots how it is done:
conservative sharp wound debridement (CSWD)
the removal of loose avascular tissue without pain or bleeding contraindications:
densely adherent necrotic tissue when interface between viable and nonviable tissue cannot be clearly identified. impaired clotting mechanism. increased risk of bleeding eg. malignant wounds. non-infected ischaemic ulcer covered with dry eschar when tissue oxygenation is insufficient to support infection control and wound healing eg. diabetic ulcers with dry gangrene
guidelines:
assess the wound and decide if CSWD is appropriate use sterile sharp instruments identify type and amount of avascular tissue to be removed be aware of underlying and adjacent anatomical structures avoid all vascular structures and any tissue not clearly identified as avascular exercise caution at periphery of wound be conservative flush the wound with sterile saline following debridement control bleeding ensure a distinct boarder between the viable & the non-viable tissue
ultrasound debridement
low frequency ultrasonic debridement (LFUD) non-invasive non-painful (although may use topical anaesthetic e. g. Emla to reduce sensitivity) minimal blood loss good wound bed preparation N/S streams through sonotrobe head with ultrasound waves, creates oscillating micro bubbles streaming steady mechanical forces wash away unhealthy tissue, also antibacterial effect healthy tissue stimulated into healing process
Skin Suture Techniques Simple, Square Interrupted Sutures… suture inserted 1cm apart & 1cm across incision
Mattress Sutures… suture inserted vertically or horizontally
Continuous Cuticular Suture…
continuous suture from start to end of the wound
Skin Staples…
metallic clips
used for primary closure
Tension Sutures… provide added support for distended abdomens or when anticipated wound breakdown
Wound Closure Strips… steri-strips non-invasive Skin Glue…
glue binds the wound together non-invasive are safe & effective method cost effective helps prevent infection ideally for wounds less than 4cm, not contaminated or infected & have skin edges that are not under tension dehiscence is slightly higher with skin glue than with sutures cosmetic outcome is comparable & it is painless contraindications for skin glue:
jagged lacerations bites, punctures or crush wounds mucosal surface axillae & perineum (high moisture areas) hands, feet & joints (unless kept dry & immobilised)
disadvantages to skin glue:
4% of wounds reopen with skin glues compared to 1-2% for sutures poor technique poor wound selection breakage of bonds & sloughing from skin...
Similar Free PDFs
Wound Care Notes Wk 3
- 14 Pages

OSCE 3 Notes - Wound Care
- 24 Pages

Wound Care Validation Notes
- 2 Pages

Wound Care
- 1 Pages

Wound modules skin care
- 2 Pages

Wound CARE FOR Diebetics
- 3 Pages

SOP WOUND CARE
- 4 Pages

Wound Care Case Study
- 4 Pages

Skills+Checklist+-+Wound+Care
- 2 Pages

Wound Care Test Bank - Potter
- 26 Pages

WK 3 - wk 3 summary
- 5 Pages

Skin Integrity and Wound Care
- 8 Pages

FHA Wound Care Pre-Lab
- 4 Pages

Wk 3 notes MBA 610
- 13 Pages
Popular Institutions
- Tinajero National High School - Annex
- Politeknik Caltex Riau
- Yokohama City University
- SGT University
- University of Al-Qadisiyah
- Divine Word College of Vigan
- Techniek College Rotterdam
- Universidade de Santiago
- Universiti Teknologi MARA Cawangan Johor Kampus Pasir Gudang
- Poltekkes Kemenkes Yogyakarta
- Baguio City National High School
- Colegio san marcos
- preparatoria uno
- Centro de Bachillerato Tecnológico Industrial y de Servicios No. 107
- Dalian Maritime University
- Quang Trung Secondary School
- Colegio Tecnológico en Informática
- Corporación Regional de Educación Superior
- Grupo CEDVA
- Dar Al Uloom University
- Centro de Estudios Preuniversitarios de la Universidad Nacional de Ingeniería
- 上智大学
- Aakash International School, Nuna Majara
- San Felipe Neri Catholic School
- Kang Chiao International School - New Taipei City
- Misamis Occidental National High School
- Institución Educativa Escuela Normal Juan Ladrilleros
- Kolehiyo ng Pantukan
- Batanes State College
- Instituto Continental
- Sekolah Menengah Kejuruan Kesehatan Kaltara (Tarakan)
- Colegio de La Inmaculada Concepcion - Cebu

